This cross-sectional, single-center study included 53 pretransplant patients for whom surgery was indicated were recruited from the ward of the liver transplantation center of Renji Hospital, Shanghai, China, from May to December 2019. Thus, this study aimed to assess the affective status, sleep quality, and daily living abilities of candidates on the OLT waiting list at a single center in China and to identify the association between these factors and disease severity as represented by the MELD score. Furthermore, the association between MELD score and sleep disturbance and daily living abilities remains unclear. 
However, more research should be done to verify the correlation between MELD scores and psychological issues. Higher posttransplant HRQOL was found in patients with a higher pretransplant MELD score. 
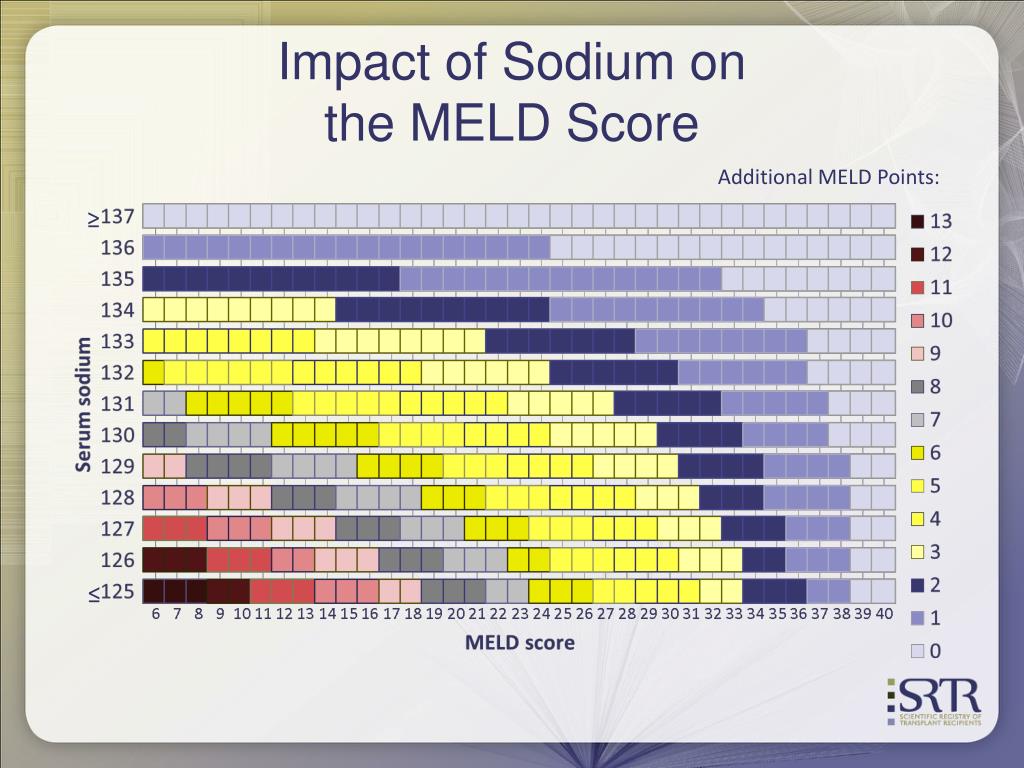
In addition to its ability to predict physiological outcomes, the MELD score also exhibits the potential to simultaneously reveal psychological outcomes in terms of health-related quality of life (HRQOL). A pretransplant MELD score of 31 to 34 predicted a 43 times greater relative life expectancy, while a MELD score of 35 to 40 had a 128 times higher expectation. A national study of the US liver transplant database revealed that a higher survival benefit was found in patients with a higher MELD score. However, an exception exists for several diseases, whereby severity is not indicated by a higher MELD score. Patients with a MELD score ≥15 are considered eligible to be placed on the waiting list. Thus, it is used as a determining factor for the OLT waiting list in accord with the idea of “the sickest first”. The MELD score has been statistically proved to predict 3-month mortality and to indicate the severity of ESLD. The model for end-stage liver disease (MELD) score was initially created to predict the survival of transjugular intrahepatic portosystemic shunts but then applied as a standard metric to reflect the severity of liver diseases. Such predictors and factors should be used as the basis for developing diagnostic and therapeutic interventions because they could help prevent the worsening of candidates’ symptoms and the negative consequences. Thus, it is important to identify the predictors of disability and the factors related to psychological disorders and sleep disturbance that could be recapitulated in the patients’ psychosocial factors. These considerations indicate a need to improve the mental and sleep status of patients. These deficits can be a predictor of mortality and, more importantly, they could determine posttransplant disability reversion for candidates on a waiting list. Functional decline, polypharmacy, and cognitive impairment, which is often seen in elderly patients, may contribute to the high risk of physical disability. Therefore, sleep disturbance appears to be a particular problem in waiting list candidates.ĭeficits in activities of daily living are common in patients with ESLD. Furthermore, sleep disturbance has a prevalence of 48% to 81% in patients with liver cirrhosis, which is much higher than in the general population. Sleep disturbance, including compromised sleep quality, has been reported among liver transplantation candidates on a waiting list. Furthermore, pretransplant depression also affects posttransplant psychiatric morbidity, while anxiety can negatively affect the course of the disease by impairing adherence to treatment. Pretransplant depression and anxiety affect posttransplant health-related quality of life (HRQOL). The prevalence rates for anxiety and depression have been estimated to be 14% to 52% and 17% to 60%, respectively. The combination of these stressors can contribute to psychological disorders such as anxiety and depression. During this time, patients face multiple stressors: declining physical health constant worry about whether the procedure will take place on time and, more importantly, in time the financial cost and so forth. However, due to the gap between supply and demand, candidates are placed on waiting lists and may have to wait for a long time before receiving the transplant. The development of orthotopic liver transplantation (OLT) has improved long-term survival and the quality of life of recipients, and the 1-, 10-, and 18-year survival rates associated with adult OLT have reached 83% to 88%, 68% to 72%, and 48% to 56%, respectively. End-stage liver disease (ESLD) not only causes severe physical deterioration, but it can also lead to psychological issues.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
